Advancements In Knee surgery and Sports Medicine
Expert Insights with:
— Mr. Sanjeev Anand —
Issue 13, March 2025

You regularly manage complex knee cases referred from other hospitals. What are some of the most challenging cases you have encountered, and how did you approach them?
In my practice, I often receive challenging cases referred from neighbouring hospitals and colleagues, which may be trauma-related, requiring urgent intervention, or complex elective pathologies requiring significant planning. Each of these cases is unique, and a standardised approach cannot be applied. Beyond the clinical challenges related to surgical management, which are often within my control, there are significant logistical challenges in organising the necessary resources to provide appropriate treatment in a timely manner. At Leeds Major Trauma Centre, we receive referrals for significant and complex knee injuries, often involving associated damage to the nerves and blood vessels, which can affect the viability of the limb. A multidisciplinary approach involving vascular surgeons and plastic surgeons is frequently required. A knee surgeon dealing with such injuries must be well-versed in 360-degree knee joint reconstruction. A substantial part of my practice is dedicated to paediatric patients, who present their own unique challenges. Knee injuries in young patients not only impact their physical health but also their mental well-being and, by extension, the welfare of their entire family. Surgical instruments are often not designed for very small knees, requiring great care and skill to prevent injury to vital structures. In my elective practice at Chapel Allerton, we receive cases with previous multiple failed surgeries, complex deformities, or severe cartilage damage in young patients. These cases require detailed preoperative assessment, multidisciplinary discussions, and meticulous planning to determine the most appropriate intervention. Postoperative rehabilitation is crucial in restoring function for these patients.
Given your specialisation in paediatric knee injuries, what are the most common misconceptions parents have about knee injuries in children?
One of the most common misconceptions is that any knee pain in a child is simply growing pains. While this is true in some cases, persistent discomfort that restricts daily activities, particularly when accompanied by joint swelling or mechanical symptoms such as locking or catching, should not be ignored. I frequently see cases where long-standing knee problems, initially dismissed as growing pains, turn out to be conditions such as osteochondritis dissecans, which require early management to prevent joint surface damage. Another common misconception is that children do not sustain serious knee injuries due to their developing musculoskeletal system. However, paediatric ACL injuries, osteochondral defects, and meniscal tears are increasingly recognised, especially in young athletes involved in high-impact sports. There is also a belief that surgery should always be delayed until skeletal maturity. While it is essential to preserve growth plates, delaying necessary surgical intervention in cases of complete ligament ruptures or unstable meniscal tears can lead to further joint damage, increasing the risk of early osteoarthritis. Additionally, some parents underestimate the importance of structured rehabilitation, assuming surgery alone will resolve the issue. In reality, a well-planned postoperative rehabilitation programme is key to a successful recovery. At other times, parents are naturally concerned about transient injuries restricting a child's physical abilities. As a surgeon, my role is to rule out serious conditions, provide reassurance, and identify issues that may benefit from early intervention to optimise function.
How do the knee problems you encounter in adolescents differ from those seen in adults, and how does this influence your treatment approach?
Knee conditions in adolescents differ from those in adults primarily due to skeletal immaturity, the presence of open growth plates, and the unique biomechanical demands of growing athletes. Unlike adults, adolescents are prone to specific injuries such as tibial spine avulsions (instead of ACL ruptures), osteochondritis dissecans, and patellar instability due to increased ligamentous laxity. Growth plate involvement necessitates specialised surgical techniques that avoid physeal damage, reducing the risk of growth disturbances. In contrast to adult knee injuries, which are often degenerative, adolescent knee injuries are frequently acute and sports-related. Treatment approaches must consider both short-term recovery and long-term joint preservation. Whenever possible, meniscal preservation is prioritised, and ACL reconstruction techniques are tailored to protect the growth plate. Young athletes are at a high risk of reinjury, so treatment strategies must aim to mitigate this risk. Another common injury pattern in sporty adolescents is repetitive stress injuries. As their skeletons mature, certain zones of weakness remain, where repetitive muscle loading can cause conditions such as Osgood-Schlatter disease or Sinding-Larsen-Johansson syndrome. It is crucial to manage activity levels in these children, as excessive demands on their growing skeletons increase their risk of injury. However, restricting them from sports can also impact their mental health. Conditions such as anterior knee pain are particularly common in adolescent girls and can significantly affect their function and psychological well-being. A holistic management approach is essential to support them through this phase while maintaining function and improving pain management.
What are the key indicators that suggest a young athlete may require surgical intervention rather than conservative treatment for a knee injury?
The decision to proceed with surgical intervention in a young athlete is based on several key indicators. These include:
- Persistent symptoms despite appropriate rehabilitation
- High-grade ligamentous injuries (such as complete ACL or PCL ruptures)
- Significant meniscal tears unlikely to heal without surgical repair
- Osteochondral injuries with loose body formation
- Recurrent episodes of joint locking or instability
Additionally, patient-specific factors such as sport-specific demands, skeletal maturity, and long-term joint preservation are critical considerations. In some cases, proactive surgery is necessary to preserve joint health, while in others, delaying surgery until skeletal maturity may be appropriate. A common injury in this age group is an anterior cruciate ligament (ACL) tear. An intact ACL is crucial not only for returning to sport but also for preventing further meniscal damage, which is vital for the long-term health of the knee joint.

Mr. Anand and team at Chapel Allerton Hospital
Could you share insights on how the field of paediatric knee surgery has evolved over the last decade?
Over the past decade, paediatric knee surgery has advanced significantly. Access to improved imaging modalities, particularly MRI, have enhanced diagnostic precision, allowing for early and accurate identification of injuries. Surgical techniques have also evolved, with a greater emphasis on reconstruction methods that preserve the native growth plate in skeletally immature patients. There is also increased awareness of meniscal preservation, with a shift towards repair rather than resection to reduce the long-term risk of osteoarthritis. Rehabilitation protocols have become more individualised, promoting a safe return to play while minimising the risk of reinjury.
You’ve been involved in developing guidelines for ACL reconstructions. What are the current best practices, and how have these changed over time?
I was fortunate to be involved in developing the BOA/BASK/BOSTAA document on “Best Practice for the Management of Anterior Cruciate Ligament (ACL) Injuries.” We are currently in the process of updating this document. Current best practices for ACL reconstruction emphasise an individualised surgical approach, appropriate graft selection, and augmentation where necessary. The transition from transtibial techniques to anteromedial portal drilling has improved tunnel positioning, enhancing graft function and reducing failure rates. There has also been a move towards early surgical intervention in high-risk populations, such as young athletes engaged in pivoting sports, to prevent secondary meniscal or cartilage damage. Additionally, there is a greater understanding of associated pathologies that must be addressed to prevent ACL reconstruction failure. Rehabilitation has evolved, with a shift from time-based to criteria-based progression, ensuring safer return to play.
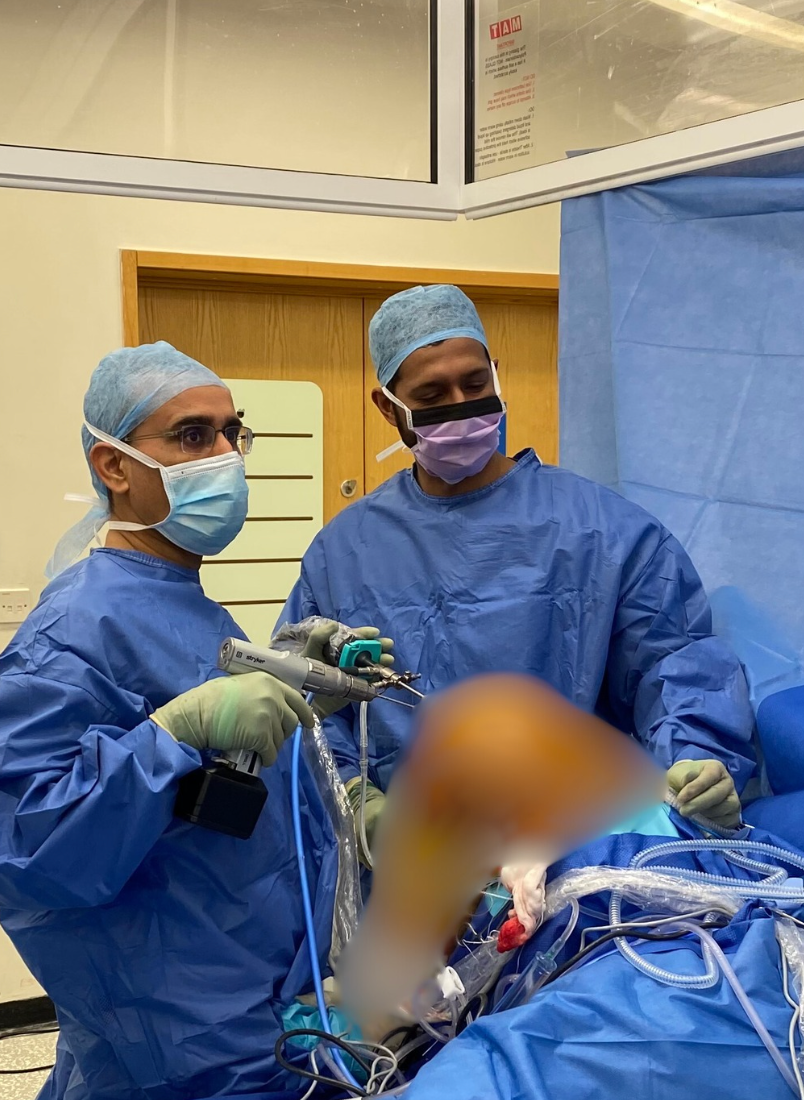
Mr. Anand teaching arthroscopy
Can you discuss your approach to managing multi-ligament knee injuries, particularly in high-performance athletes?
Management of multi-ligament knee injuries in high-performance athletes requires a systematic and individualised approach. Surgical timing is critical, with staged versus single-stage reconstruction decisions based on the severity of soft tissue injury and neurovascular involvement. Anatomical reconstruction of all injured ligaments, rather than non-anatomic repair, is preferred to optimise stability and function. Rehabilitation protocols are structured to restore neuromuscular control while preventing stiffness. Close collaboration with physiotherapists is essential to a safe and efficient return to competition. Though this is a rare injury, with our major trauma service, we do receive a good number of these patients and have been fortunate to develop expertise in their management. These are complex injuries and are best dealt with in specialist units with multidisciplinary input available.
What gaps do you currently see in research related to knee injuries in young athletes, and what areas would you like to explore further?
I was part of a working group which led on identifying the top 10 research priorities in first-time soft tissue knee injuries, in partnership with the James Lind Alliance. This document is important as it looks at research questions that are meaningful to patients. Appropriate timing and management strategies for soft tissue knee injuries remain a critical concern. There are several gaps in research surrounding knee injuries in young athletes. Firstly, long-term outcomes following paediatric ACL reconstruction, particularly regarding re-injury rates and post-traumatic osteoarthritis, require further study. Additionally, there is a need for improved understanding of optimal rehabilitation strategies to reduce failure rates. The role of biologics and tissue engineering in enhancing graft healing and meniscal repair outcomes is another promising area for future research. Finally, developing better injury prevention programs tailored to different sports and age groups remains a priority.
Given your role as a trainer for arthroscopy skills, what do you believe are the key skills new orthopaedic surgeons must master early in their careers?
Mastery of arthroscopy requires a combination of technical proficiency, spatial awareness, and decision-making skills. Early-career surgeons must develop strong hand-eye coordination and dexterity to handle instruments efficiently within a confined joint space. Understanding triangulation and portal placement is crucial for optimising visualisation. In addition, they should focus on performing diagnostic arthroscopy with precision before progressing to more complex procedures such as meniscal repair and ligament reconstruction. Simulation training and cadaveric workshops play a vital role in refining these skills before transitioning to live surgery. I was part of a group that ran an arthroscopy course at the Royal College of Surgeons of England for many years. Now, in my role as Education Secretary for BOSTAA, I help with organising cadaveric courses for the next generation of surgeons.
How do you integrate your clinical experiences into your teaching curriculum for orthopaedic trainees?
Integrating clinical experience into teaching involves a combination of case-based learning, hands-on surgical training, and structured mentorship. At Leeds, we have a long-running knee fellowship programme, training soft tissue knee surgeons for the future. To my fellows, I emphasise the importance of understanding patient-specific factors in surgical decision-making, reinforcing this through case discussions and intraoperative teaching. Additionally, I encourage trainees to engage in research projects that bridge clinical practice with evidence-based improvements. Regular assessment and feedback help trainees refine their skills and develop confidence in their surgical approach.
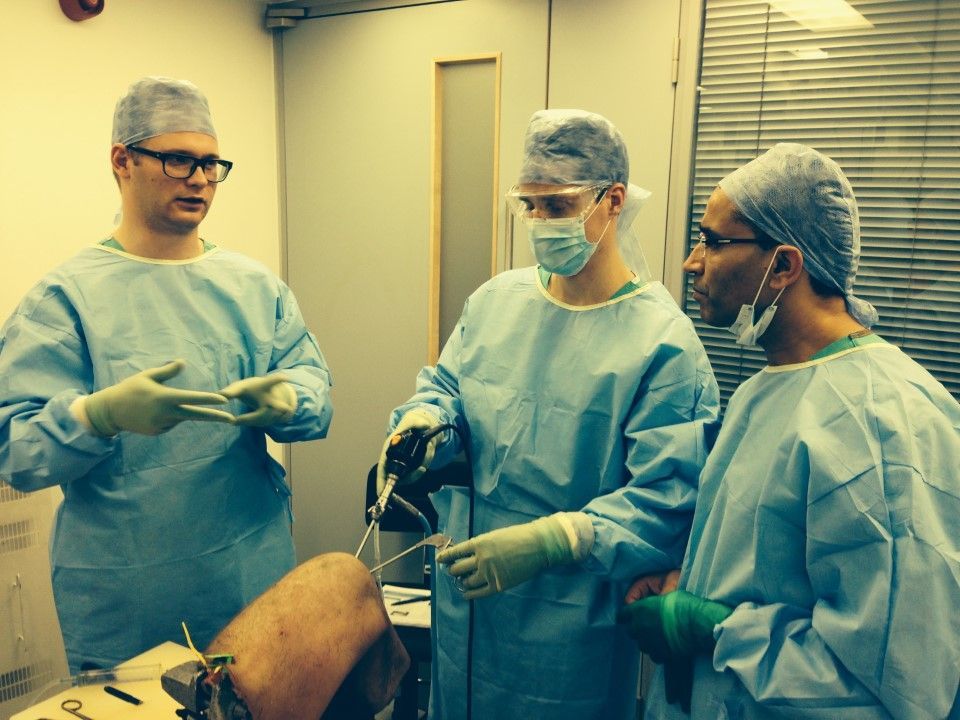
Mr. Anand teaching on a surgical skills course
As a founder member and Academic Chair of ISKSAA, what are your primary goals for the organisation in the coming years?
I have been involved with ISKSAA soon after its inception. My main role has been in delivering its fellowship programme besides working as editor for its journal. I have now given up my work for the journal but am still coordinating the fellowship programme. These fellowships help improve standards of care for our patients by exchanging best practices across countries. We have placed nearly 300 fellows in different centres across the world since 2013. The primary goals for ISKSAA in the coming years include expanding opportunities for international fellowships, fostering collaborative research in sports medicine, and enhancing access to high-quality education through digital platforms. We aim to strengthen partnerships with global orthopaedic societies to facilitate knowledge exchange. We are hosting Great North Debate (www.greatnorthdebate.com) in Leeds in June 2025, in partnership with ISKSAA. We have an excellent faculty and scientific programme and would love to see you all in Leeds.
What advice would you give to medical students or junior doctors considering a career in orthopaedic surgery, particularly in sports injuries?
For those considering a career in orthopaedic surgery, I recommend developing a strong foundation in anatomy, biomechanics, and clinical assessment early on. Exposure to sports injuries through observerships and research projects can provide valuable insights. Additionally, acquiring surgical skills through cadaveric courses and simulation training is beneficial. It is crucial to stay updated with emerging techniques and actively engage in mentorship programs to refine both technical and decision-making abilities.
How has international collaboration through platforms like ISKSAA influenced surgical techniques and knowledge exchange in your experience?
International collaboration has significantly enhanced the exchange of surgical techniques, research advancements, and best practices. Through ISKSAA, we have facilitated international fellowships that allow surgeons to gain exposure to diverse approaches and cutting-edge technologies. Collaborative research initiatives have also contributed to the refinement of surgical protocols, improving patient outcomes. The ability to share complex cases and discuss management strategies with experts worldwide has been invaluable in advancing orthopaedic sports medicine.
The value of these international collaborations is recognised by surgeons across the world. I was fortunate to be awarded BASK’s Presidential Medal in 2023 for my work in fostering these collaborations.
What future trends or innovations do you anticipate will reshape the field of orthopaedic sports medicine over the next decade?
Several innovations are likely to reshape orthopaedic sports medicine in the coming decade. Advances in biologic therapies, including stem cell-based treatments, may enhance tissue healing and regeneration. Robotics and artificial intelligence will further refine surgical precision and decision-making. Additionally, improved wearable technology and motion analysis systems will play a greater role in injury prevention and rehabilitation. Personalised medicine, including genetic profiling for injury risk stratification, may also become an integral part of athlete management.
About Mr. Sanjeev Anand

Mr Anand has a special interest in treating all aspects of knee problems from sports injuries to arthritic knees. As a surgeon practising at a tertiary referral centre, a major part of his practice involves managing complex problems referred from colleagues and neighbouring hospitals. He also regularly treats paediatric knee problems both in the NHS and in the private sector. He is a recognised expert in treating Anterior Cruciate ligament injuries and led a working group that wrote national guidelines on ACL reconstruction. He has extensive experience in dealing with complex knee injuries requiring the reconstruction of multiple injured structures in the knee joint. His surgical approach is to preserve joint surface and meniscus to maximise function. He was part of the group which developed national guidelines for arthroscopic knee surgery. If an arthritic joint cannot be preserved, he offers a range of knee replacement options using the latest techniques. He holds weekly acute knee injury clinics at Nuffield Health Leeds Hospital to ensure prompt and optimum treatment for often missed injuries. He also has extensive experience in hip arthroscopic surgery, to deal with selected groin pain conditions and trochanteric bursitis. Mr Anand trained in Orthopaedics in London, Manchester and Leeds. Upon completion of his UK orthopaedic training, he undertook Specialist Surgical Fellowship training in arthroplasty and sports injuries in Australia. He is a trainer for arthroscopy skills and regularly conducts workshops for orthopaedic trainees. He is a founding member and Executive Director of the International Society for Knowledge for Surgeons on Arthroscopy and Arthroplasty (ISKSAA) and is Executive editor of the Journal of Arthroscopy and Joint Surgery. In 2023, Mr Anand was awarded the British Association for Surgery of the Knee President’s medal. He currently holds the position of Academic Secretary to the British Orthopaedic Sports Trauma and Arthroscopy Association (BOSTAA)." Find out more about Mr Sanjeev Anand, visit his website: kneeandsportsurgery.co.uk
We would like to thank Mr. Sanjeev Anand for his time and insight into orthopaedic excellence.
Thank You for being part of Our Community
We believe in pushing boundaries, sharing knowledge, and highlighting the people and ideas shaping the future.
On The Podium is our platform for showcasing the journeys, challenges, and breakthroughs of those making an impact in space, technology, and beyond.
If you’ve found value in these stories, we encourage you to stay connected. Follow us on social media for the latest updates, subscribe to our email list for exclusive content, and share these insights with others who might find them just as inspiring. Your engagement helps us continue to bring important stories to light and grow a community of forward thinkers.
Thank you for reading, supporting, and being part of this journey. We look forward to exploring more with you.
Thank you to our sponsors:
To download this issue of On The Podium, click below.

Sign up to On The Podium. The latest insights and inspiration from orthopaedic specialists around the globe sent straight to your inbox.
On The Podium
The newsletter brought to you by OrthoSpaceX
| Engage with Orthopaedic Leaders | Exclusive orthopaedic insight | |
| Stay Ahead in Orthopaedic Advancements | Uncover Surgical Innovations | |
| Empower Your Orthopaedic Knowledge | Unlock the Minds of Orthopaedic Specialists |

Slide title
Write your caption hereButton
Slide title
Write your caption hereButtonSlide title
Write your caption hereButtonSlide title
Write your caption hereButtonSlide title
Write your caption hereButton
Slide title
Write your caption hereButton
Thank you for subscribing
Please try again later.







